|
Schizophrenia Treatment & CausesThinking About Becoming A Psychology Student? Find A Psychology School Near YouSchizophrenia Treatment & Causes
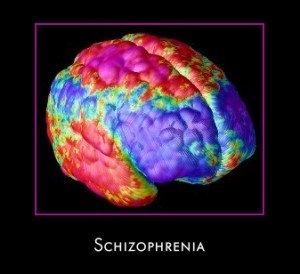
The following information is provided courtesy of The National Institute of mental Health. What Causes Schizophrenia?Like many other illnesses, schizophrenia is believed to result from a combination of environmental and genetic factors. All the tools of modern science are being used to search for the causes of this disorder. Can schizophrenia be Inherited? Scientists have long known that schizophrenia runs in families. It occurs in 1 percent of the general population but is seen in 10 percent of people with a first-degree relative (a parent, brother, or sister) with the disorder. People who have second-degree relatives (aunts, uncles, grandparents, or cousins) with the disease also develop schizophrenia more often than the general population. The identical twin of a person with schizophrenia is most at risk, with a 40 to 65 percent chance of developing the disorder. Our genes are located on 23 pairs of chromosomes that are found in each cell. We inherit two copies of each gene, one from each parent. Several of these genes are thought to be associated with an increased risk of schizophrenia, but scientists believe that each gene has a very small effect and is not responsible for causing the disease by itself. It is still not possible to predict who will develop the disease by looking at genetic material. Although there is a genetic risk for schizophrenia, it is not likely that genes alone are sufficient to cause the disorder. Interactions between genes and the environment are thought to be necessary for schizophrenia to develop. Many environmental factors have been suggested as risk factors, such as exposure to viruses or malnutrition in the womb, problems during birth, and psychosocial factors, like stressful environmental conditions. Do people with schizophrenia have faulty brain chemistry? It is likely that an imbalance in the complex, interrelated chemical reactions of the brain involving the neurotransmitters dopamine and glutamate (and possibly others) plays a role in schizophrenia. Neurotransmitters are substances that allow brain cells to communicate with one another. Basic knowledge about brain chemistry and its link to schizophrenia is expanding rapidly and is a promising area of research. Do the brains of people with schizophrenia look different? The brains of people with schizophrenia look a little different than the brains of healthy people, but the differences are small. Sometimes the fluid-filled cavities at the center of the brain, called ventricles, are larger in people with schizophrenia; overall gray matter volume is lower; and some areas of the brain have less or more metabolic activity. Microscopic studies of brain tissue after death have also revealed small changes in the distribution or characteristics of brain cells in people with schizophrenia. It appears that many of these changes were prenatal because they are not accompanied by glial cells, which are always present when a brain injury occurs after birth. One theory suggests that problems during brain development lead to faulty connections that lie dormant until puberty. The brain undergoes major changes during puberty, and these changes could trigger psychotic symptoms. The only way to answer these questions is to conduct more research. Scientists in the United States and around the world are studying schizophrenia and trying to develop new ways to prevent and treat the disorder. Schizophrenia TreatmentBecause the causes of schizophrenia are still unknown, current treatments focus on eliminating the symptoms of the disease. Schizophrenia Treatment: Antipsychotic Medications Antipsychotic medications have been available since the mid-1950s. They effectively alleviate the positive symptoms of schizophrenia. While these drugs have greatly improved the lives of many patients, they do not cure schizophrenia. Everyone responds differently to antipsychotic medication. Sometimes several different drugs must be tried before the right one is found. People with schizophrenia should work in partnership with their doctors to find the medications that control their symptoms best with the fewest side effects. The older antipsychotic medications include chlorpromazine (Thorazine), haloperidol (Haldol), perphenazine (Etrafon, Trilafon), and fluphenzine (Prolixin). The older medications can cause extrapyramidal side effects, such as rigidity, persistent muscle spasms, tremors, and restlessness. In the 1990s, new drugs, called atypical antipsychotics, were developed that rarely produced these side effects. The first of these new drugs was clozapine (Clozaril). It treats psychotic symptoms effectively even in people who do not respond to other medications, but it can produce a serious problem called agranulocytosis, a loss of the white blood cells that fight infection. Therefore, patients who take clozapine must have their white blood cell counts monitored every week or two. The inconvenience and cost of both the blood tests and the medication itself has made treatment with clozapine difficult for many people, but it is the drug of choice for those whose symptoms do not respond to the other antipsychotic medications, old or new. Some of the drugs that were developed after clozapine was introduced—such as risperidone (Risperdal), olanzapine (Zyprexa), quietiapine (Seroquel), sertindole (Serdolect), and ziprasidone (Geodon)—are effective and rarely produce extrapyramidal symptoms and do not cause agranulocytosis; but they can cause weight gain and metabolic changes associated with an increased risk of diabetes and high cholesterol. People respond individually to antipsychotic medications, although agitation and hallucinations usually improve within days and delusions usually improve within a few weeks. Many people see substantial improvement in both types of symptoms by the sixth week of treatment. No one can tell beforehand exactly how a medication will affect a particular individual, and sometimes several medications must be tried before the right one is found. When people first start to take atypical antipsychotics, they may become drowsy; experience dizziness when they change positions; have blurred vision; or develop a rapid heartbeat, menstrual problems, a sensitivity to the sun, or skin rashes. Many of these symptoms will go away after the first days of treatment, but people who are taking atypical antipsychotics should not drive until they adjust to their new medication. If people with schizophrenia become depressed, it may be necessary to add an antidepressant to their drug regimen. Length of Schizophrenia Treatment Like diabetes or high blood pressure, schizophrenia is a chronic disorder that needs constant management. At the moment, it cannot be cured, but the rate of recurrence of psychotic episodes can be decreased significantly by staying on medication. Although responses vary from person to person, most people with schizophrenia need to take some type of medication for the rest of their lives as well as use other approaches, such as supportive therapy or rehabilitation. Relapses occur most often when people with schizophrenia stop taking their antipsychotic medication because they feel better, or only take it occasionally because they forget or don't think taking it regularly is important. It is very important for people with schizophrenia to take their medication on a regular basis and for as long as their doctors recommend. If they do so, they will experience fewer psychotic symptoms. No antipsychotic medication should be discontinued without talking to the doctor who prescribed it, and it should always be tapered off under a doctor's supervision rather than being stopped all at once. There are a variety of reasons why people with schizophrenia do not adhere to treatment. If they don't believe they are ill, they may not think they need medication at all. If their thinking is too disorganized, they may not remember to take their medication every day. If they don't like the side effects of one medication, they may stop taking it without trying a different medication. Substance abuse can also interfere with treatment effectiveness. Doctors should ask patients how often they take their medication and be sensitive to a patient's request to change dosages or to try new medications to eliminate unwelcome side effects. There are many strategies to help people with schizophrenia take their drugs regularly. Some medications are available in long-acting, injectable forms, which eliminate the need to take a pill every day. Medication calendars or pillboxes labeled with the days of the week can both help patients remember to take their medications and let caregivers know whether medication has been taken. Electronic timers on clocks or watches can be programmed to beep when people need to take their pills, and pairing medication with routine daily events, like meals, can help patients adhere to dosing schedules. Schizophrenia Treatment: Medication Interactions Antipsychotic medications can produce unpleasant or dangerous side effects when taken with certain other drugs. For this reason, the doctor who prescribes the antipsychotics should be told about all medications (over-the-counter and prescription) and all vitamins, minerals, and herbal supplements the patient takes. Alcohol or other drug use should also be discussed. Schizophrenia Treatment: Psychosocial Treatment Numerous studies have found that psychosocial treatments can help patients who are already stabilized on antipsychotic medications deal with certain aspects of schizophrenia, such as difficulty with communication, motivation, self-care, work, and establishing and maintaining relationships with others. Learning and using coping mechanisms to address these problems allows people with schizophrenia to attend school, work, and socialize. Patients who receive regular psychosocial treatment also adhere better to their medication schedule and have fewer relapses and hospitalizations. A positive relationship with a therapist or a case manager gives the patient a reliable source of information, sympathy, encouragement, and hope, all of which are essential for for managing the disease. The therapist can help patients better understand and adjust to living with schizophrenia by educating them about the causes of the disorder, common symptoms or problems they may experience, and the importance of staying on medications. Schizophrenia Treatment: Illness Management Skills People with schizophrenia can take an active role in managing their own illness. Once they learn basic facts about schizophrenia and the principles of schizophrenia treatment, they can make informed decisions about their care. If they are taught how to monitor the early warning signs of relapse and make a plan to respond to these signs, they can learn to prevent relapses. Patients can also be taught more effective coping skills to deal with persistent symptoms. Schizophrenia Treatment: Integrated Treatment for Co-occurring Substance Abuse Substance abuse is the most common co-occurring disorder in people with schizophrenia, but ordinary substance abuse treatment programs usually do not address this population's special needs. Integrating schizophrenia treatment programs and drug treatment programs produces better outcomes. Schizophrenia Treatment: Rehabilitation Rehabilitation emphasizes social and vocational training to help people with schizophrenia function more effectively in their communities. Because people with schizophrenia frequently become ill during the critical career-forming years of life (ages 18 to 35) and because the disease often interferes with normal cognitive functioning, most patients do not receive the training required for skilled work. Rehabilitation programs can include vocational counseling, job training, money management counseling, assistance in learning to use public transportation, and opportunities to practice social and workplace communication skills. Schizophrenia Treatment: Family Education Patients with schizophrenia are often discharged from the hospital into the care of their families, so it is important that family members know as much as possible about the disease to prevent relapses. Family members should be able to use different kinds of treatment adherence programs and have an arsenal of coping strategies and problem-solving skills to manage their ill relative effectively. Knowing where to find outpatient and family services that support people with schizophrenia and their caregivers is also valuable. Schizophrenia Treatment: Cognitive Behavioral Therapy Cognitive behavioral therapy is useful for patients with symptoms that persist even when they take medication. The cognitive therapist teaches people with schizophrenia how to test the reality of their thoughts and perceptions, how to "not listen" to their voices, and how to shake off the apathy that often immobilizes them. This treatment appears to be effective in reducing the severity of symptoms and decreasing the risk of relapse. Schizophrenia Treatment: Self-Help Groups Self-help groups for people with schizophrenia and their families are becoming increasingly common. Although professional therapists are not involved, the group members are a continuing source of mutual support and comfort for each other, which is also therapeutic. People in self-help groups know that others are facing the same problems they face and no longer feel isolated by their illness or the illness of their loved one. The networking that takes place in self-help groups can also generate social action. Families working together can advocate for research and more hospital and community treatment programs, and patients acting as a group may be able to draw public attention to the discriminations many people with mental illnesses still face in today's world. Support groups and advocacy groups are excellent resources for people with many types of mental disorders. More Schizophrenia InformationSee following link for information on what schizophrenia is, schizophrenia symptoms, onset & schizophrenia & violence. Essential Schizophrenia ReadingDiagnosis: Schizophrenia by Professor Rachel Miller & Professor Susan Mason
Book Description Now in a revised and expanded third edition, this handbook presents the latest knowledge on the nature, diagnosis, assessment, and treatment of Attention-Deficit/Hyperactivity Disorder (ADHD). Provided are state-of-the-art guidelines for understanding and managing the challenges ADHD poses to children, adolescents, and adults in a range of settings. Featuring a new chapter on combined therapies, this book is the most comprehensive, authoritative, and up-to-date work in the field. See following link for more details: Classic Articles All Psychology Students Should Read
This special Kindle collection consists of the most influential, infamous and iconic research articles ever published in the history of psychology. See following link for full details. The Psychology Classics Kindle Collection Go Back To The Main Mental Health Page Go From Schizophrenia Treatment Back To The Home Page
|